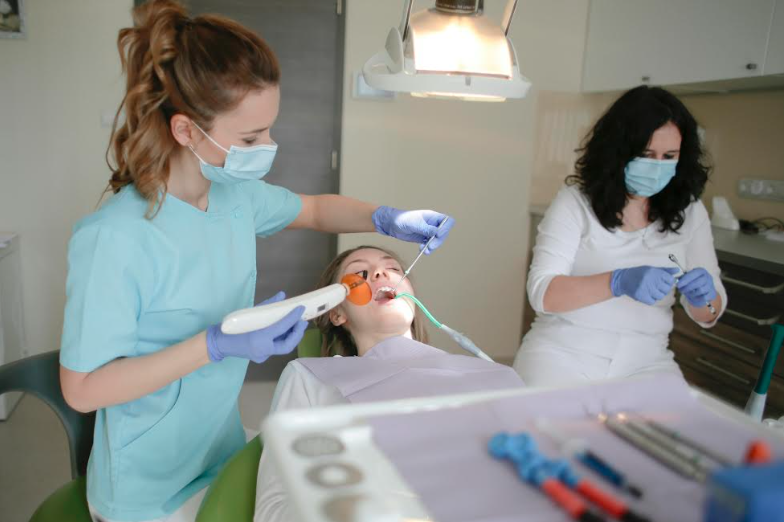
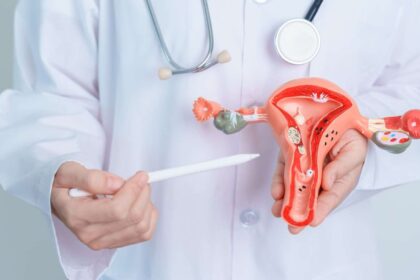
Oral health doesn’t usually come up when talking about reproductive health, as the relationship between oral health and reproductive outcomes is often underestimated. Dentistry and gynecology are typically treated as separate domains, yet there’s increasing attention on how gum health and low-grade inflammation in the mouth can influence the rest of the body. Emerging clinical evidence shows a measurable connection between periodontal health and conditions such as preterm birth, low birth weight, and systemic inflammation.
Preventive dental care, in this context, isn’t about appearance or smile. It’s about reducing a source of inflammation that the body would otherwise keep dealing with in the background.
How Your Mouth And Reproductive Health Are Secretly Linked
Your bloodstream is basically the main transport route. When gum disease reaches the periodontitis stage, your immune system starts sending out inflammatory messengers (interleukin-6 and TNF-alpha). Those messengers don’t stay in your mouth; they travel everywhere and can gently mess with ovulation timing, how an embryo implants, or even how the placenta develops.
The European Federation of Periodontology’s October 2025 summary on periodontal diseases in women across life stages really spells it out, especially during pregnancy, when hormones make gums way more reactive.
If there’s already periodontitis in the picture, it often lines up with modestly higher risks for preterm birth, low birth weight, preeclampsia, and gestational diabetes. They also mention that poor periodontal health might play a role in some cases of female infertility, though they’re careful to say we still need bigger, better studies to be sure how strong that link really is.
Bottom line: extra immune noise and oxidative stress are adding stress to the reproductive system that it didn’t sign up for.
Hormones Make Things Less Predictable
Hormonal changes don’t just affect energy levels or mood. They change how the body reacts to plaque and bacteria.
During pregnancy, for example, gums tend to become more reactive. Something minor can suddenly look worse, such as swelling, bleeding, or sensitivity. It’s not necessarily poor hygiene. It’s the body responding differently.
Saliva changes too, slightly altering the bacterial environment. Nothing extreme, but enough to shift the balance if oral care slips even a little. On their own, these changes aren’t alarming. The issue is how quickly small gaps in care can turn into bigger problems under these conditions.
Prevention Is Boring, but It Works
Preventive care doesn’t feel urgent. That’s why it’s often delayed. But this is where most of the actual benefit sits. Regular check-ups catch inflammation early. Cleanings remove buildup that brushing can’t. Small adjustments, such as timing, technique, and even diet, make a noticeable difference over time. It’s not complicated. It’s just consistent. And that’s the part people struggle with.
Choosing Care That Actually Aligns
Not all dental care is approached the same way. Some clinics focus purely on treatment. Others take a broader view, connecting oral health with overall wellbeing. That difference matters more than it seems.
When choosing a provider, factors like location and convenience still matter. But there’s also a shift toward clinics that understand the bigger picture. For example, someone might choose a Kensington dentist if the goal is ongoing, preventive care that aligns with long-term health, not just quick fixes.
Healthcare Is Slowly Connecting the Dots
There’s a gradual move toward more integrated healthcare. Different specialities are starting to overlap instead of operating in isolation. Dentistry is part of that shift, even if it’s happening quietly.
For women, this changes how preventive care should be viewed. Oral health isn’t separate. It sits alongside other factors that influence hormones, inflammation, and overall stability. Ignoring it doesn’t make things simpler. It just delays when the problem shows up.
Final Take
Preventive dental care is easy to push aside because it doesn’t feel urgent until it is. By the time discomfort appears, the issue has usually been there for a while. And sometimes, it’s already affecting more than expected.
A more practical approach is to treat oral health as part of the bigger picture. Not something extra. Not something optional. The connection to reproductive health isn’t dramatic or obvious, as it builds slowly, in the background. That’s exactly why it tends to be overlooked and exactly why it shouldn’t be.